September is Ovarian Cancer Awareness Month and bringing awareness to this silent killer became particularly important to me when I lost my mom to ovarian cancer back in 2016.
Watching her health deteriorate and feeling helpless as she ultimately lost her battle with ovarian cancer was devastating. My hope is that by sharing information about what might increase the risk of developing this type of cancer, as well as what signs to look for, more women’s lives can be spared.
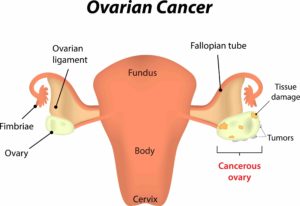
The reason ovarian cancer is sometimes referred to as a “silent killer” is that in its early stages, it can be very difficult to detect. Ovarian cancer begins in the ovaries and eventually spreads to the pelvis and abdomen. Most women rarely experience symptoms before it spreads and becomes deadly.
When the cancer is confined to the ovaries, surgery to remove it and/or chemotherapy treatment is likely to be successful. Ovarian cancer is much more difficult to treat and becomes most dangerous once it has spread into other areas.
There are three different types of ovarian cancer: stromal tumors, epithelial tumors, and germ cell tumors.
The type of ovarian cancer is determined by the type of cell in which it originates. For example, stromal tumors originate in the ovarian tissue, housing an array of hormone-producing cells. However, only about seven percent of ovarian tumors are stromal. There are also epithelial tumors. This is the most common type of ovarian cancer, making up about 90 percent of all ovarian cancers. These tumors begin in thin tissue outside the ovaries. Finally, there are germ cell tumors; the rarest form of ovarian cancer. Originating in the egg-producing cells, germ cell tumors are most often seen in younger women.
According to the Centers for Disease Control, 21,000 women each year will be diagnosed with ovarian cancer and 14,000 will die from the disease.
So, how do you assess your risk for developing ovarian cancer? First of all, if you have a family history of ovarian or breast cancer (especially if two or more close relatives have had either of these diseases), set up an appointment with your doctor to discuss any questions or concerns. They may recommend a genetic counselor who can test for gene mutations that increase your risk of developing either of these types of cancer.
Inherited gene mutations on the BRCA1 and BRCA2 genes can increase your risk of developing ovarian or breast cancer. The good news is, testing positive for either of these mutations isn’t inevitably a death sentence.
 My decision to undergo a full hysterectomy and oophorectomy, as well as a double mastectomy after my positive BRCA test, was a difficult one to make. However, seeing the toll treatment for ovarian cancer took on my mom, and then to have her lose her battle with the disease made me realize it was the best only option.
My decision to undergo a full hysterectomy and oophorectomy, as well as a double mastectomy after my positive BRCA test, was a difficult one to make. However, seeing the toll treatment for ovarian cancer took on my mom, and then to have her lose her battle with the disease made me realize it was the best only option.
As I mentioned above, there are few (if any) symptoms of ovarian cancer before it spreads but be sure to talk to your doctor if you experience any of the following symptoms:
- Irregularity in bowel movements, such as constipation
- Decreased appetite
- Weight loss
- Frequent urination
- Abdominal bloating/swelling
- Pelvic discomfort
Other risk factors like early menses or late onset of menopause can also increase your chances of developing ovarian cancer. Estrogen hormone replacement therapy over extended periods of time or in large doses has also been shown to increase your risk as well.
Ovarian cancer occurs most often in women who are 50-60 years old, however, it can occur in younger women. Understanding the risk factors will help you gauge whether or not you should look into testing.
Ovarian cancer can be difficult to understand and navigate because symptoms in the early stages are so rare. But it’s important to know that you do have options. Don’t hesitate to schedule an appointment with your doctor if you’re aware of a family history of the disease or if you have any indication that you might be at risk.